The Seductive Allure of the E-Patient
New columnist Paul Ivsin charts the rise of the e-patient & the future of patient-assisted trial design.

Following e-patients through social media is as close as I get to celebrity-watching. While I just can’t seem to get myself excited about which basketball player is dating which actress, or what the billionaire’s son got arrested for this time, I spend hours each week reading – and occasionally directly engaging with – that fascinating group of people who have come forward to document and discuss their experiences with their illnesses and treatments. The 21st century e-patient is not just a disease advocate attending fundraisers and raising awareness, but an active chronicler providing a vividly 3-dimensional portrait of their condition and its impact on their life.
Of the few e-patients who frequently engage on the specific topic of clinical trials, two of my most-watched favorites are Jeri Burtchell and Jack Whelan. While they haven’t yet reached Kardashian status, both have achieved a level of microcelebrity in the clinical research world: pharma companies follow them on Twitter and invite them to speak frequently at industry conferences.
 … As well they should. I was a fan of Jeri’s the moment I read “A hypochondriac joins a clinical trial”. The first time I saw Jack in person, he was giving a polite but well-sharpened piece of his mind to the leader of a Federal research institute. As far as I’m concerned, their work is required reading for anyone serious about improving clinical trials. They’re thoughtful, articulate, and always engaged.
… As well they should. I was a fan of Jeri’s the moment I read “A hypochondriac joins a clinical trial”. The first time I saw Jack in person, he was giving a polite but well-sharpened piece of his mind to the leader of a Federal research institute. As far as I’m concerned, their work is required reading for anyone serious about improving clinical trials. They’re thoughtful, articulate, and always engaged.
And they’re only the most visible tip of the e-patient iceberg. There are thousands of people taking to the web to share, discuss, and opine on every healthcare topic, and their numbers are growing rapidly.
The Voice of the Patient in Protocol Design
Everyone wants to run trials that enroll patients quickly. That means understanding how patients will view the trial when trying to decide whether to enroll. It’s important for us to ask concrete questions that can have a direct impact on protocol design, such as:
- How do they view the extra visits? What’s preferable: fewer, longer visits or more frequent but shorter visits?
- How tolerant are they of trial procedures – blood draws, imaging, etc.? Will too many of these discourage otherwise-interested patients?
- What kinds of patients are most actively looking for new options? Where are they going for information?
E-patients give us an exciting new way to answer these questions. We can bring on an individual e-patient advisor to the protocol team, providing ongoing perspective as the trial moves from concept to synopsis to first draft. Or, we can implement a social listening program to trawl through the oceans of online discussions and bring common themes, concerns, and attitudes to the surface.
Which Voice? Which Patient?
But here’s the dilemma: insofar as e-patients are distinctive, they are also unrepresentative. The very qualities that make them worth listening to are also qualities that make them different from other patients – and those other patients are the ones you will likely need for your trial. Most trial patients are not going to have Jeri’s meticulous attention to detail, or Jack’s nonstop determination. In all likelihood, they’re going to be a lot more hesitant and confused about the opportunity to be in a trial.
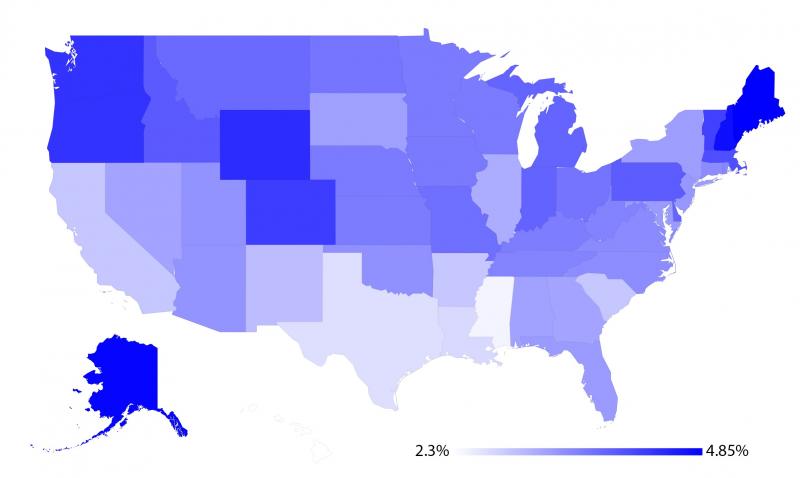
This applies to the broader e-patient community as well. A new study published in this month’s issue of the Journal of Medical Internet Research makes an important effort towards quantifying the mismatch between e-patients and all patients. Looking both at social networks such as Twitter and Google+, as well as health-focused discussion forums and drug review websites, the study team collected and modeled the demographics of engaged internet users.
As a whole, the study found that e-patients in the US varied considerably from the general population. Compared with adults in the US as a whole, e-patients were:
- Younger
- Wealthier
- More educated
- Less ethnically diverse
These are many of the same disparities that already exist in clinical trial participation, and which therefore already exacerbate low enrollment rates.
The danger here is clear: the value that e-patients bring may be undermined by the fact that their demographics tend to skew away from exactly those populations we’d like to engage more fully in clinical trials.
(One interesting exception to this, I’ll note, is women. Historically underrepresented in clinical trials, women predominate in online engagement, making up more than three-fourths of the user base of drug review sites and health forums. So paying attention to online discussions may provide some immediate benefit by increasing the volume of female voices heard.)
Not only can listening to the e-patient community give us an unrepresentative sample of patient perspectives, but the qualitative nature of much patient-centered trial design will sometimes lend itself to vague conclusions and unjustified interpretations. It is unfortunately very easy to grab onto a particular e-patient perspective if it happens to already align with ours, or we may try too hard to fit patient feedback into our needs (for example, interpreting discontent with current medications as a willingness to switch to a trial, when in fact it may signal something else, such as a strained doctor/patient relationship).
The Future of Patient-Assisted Trial Design
The use of patient advisors and social media listening represents an important advance in how we design our trials. Prior to this, trial teams often simply resorted to speculation about “what patients want” – or, sometimes worse, relied on physician opinion leaders to tell them what patients were thinking. We are much better off with e-patient input than without it, but pitfalls remain.
So what is the best way forward? Part of the problem will start to solve itself over time: as more people become comfortable engaging on health topics online, the e-patient community will grow and naturally become more diverse and representative. Until then, we need to augment our patient input by engaging underrepresented patients – many of these can be found through more direct tools such as structured surveys and interviews.
Ultimately, however, a truly patient-centric approach will need to integrate qualitative e-patient insights with robust quantitative data. Potential trial participants are a heterogeneous group, and individual anecdotes need to be balanced by careful analysis of demographic and medical data.
None of this, obviously, should deter anyone from listening to and engaging with the e-patient community. The very fact that we have, for the first time, such an opportunity to tap into patients makes this a truly exciting time to be involved in clinical research. But it will benefit us to pause and understand what this opportunity brings us, what it doesn’t, and what still remains to be done.
Paul Ivsin is the Offerings Director for the Clinical Trial Optimization Solutions unit of IMS Health, where he focuses on bringing patient-focused tools to pharmaceutical clinical trials. A renowned expert on study enrollment strategies and patient engagement, he also writes on clinical trial issues at his blog Placebo Control.
Patient-Centered Clinical Trials USA 2015
Boost Clinical Trial Productivity – Collaborate with Patients at the Heart of your Research.

